-
- Find Care
-
- Visitor Information
- Find a Location
- Shuttles
- Visitor Policies
-
-
- Our Virtual Care Options
- 24/7 Virtual Care
- Virtual Visits for Primary & Specialty Care
- Online Second Opinions
- Participate in Research
-
- Contact us
-
- For Innovators
- Commercialization Guide for Innovators
-
-
- Research News
- Alzheimer's Disease
- Artificial Intelligence
-
- Overview
-
- Overview
- Getting Started
- New to Mass General Brigham
- International Patient Services
- What Is Patient Gateway?
- Planning Your Visit
- Find a Doctor (opens link in new tab)
- Appointments
- Patient Resources
- Health & Wellness
- Flu, COVID-19, & RSV
- Billing & Insurance
- Financial Assistance
- Medicare and MassHealth ACOs
- Participate in Research
- Educational Resources
- Visitor Information
- Find a Location
- Shuttles
- Visitor Policies
- Find Care
-
- Overview
- Our Virtual Care Options
- 24/7 Virtual Care
- Virtual Visits for Primary & Specialty Care
- Online Second Opinions
-
- Overview
- Participate in Research
-
- Overview
- About Innovation
- About
- Team
- News
- For Industry
- Venture Capital and Investments
- World Medical Innovation Forum (opens link in new tab)
- Featured Licensing Opportunities
- For Innovators
- Commercialization Guide for Innovators
- Contact us
-
- Overview
- Information for Researchers
- Compliance Office
- Research Cores
- Clinical Trials
- Advisory Services
- Featured Research
- Two Centuries of Breakthroughs
- Advances in Motion (opens link in new tab)
- Brigham on a Mission (opens link in new tab)
- Gene and Cell Therapy Institute
- Research News
- Alzheimer's Disease
- Artificial Intelligence
-
- Overview
-
- Overview
- Residency & fellowship programs
- Brigham and Women's Hospital
- Massachusetts General Hospital
- Mass Eye and Ear
- Newton-Wellesley Hospital
- Salem Hospital
- Integrated Mass General Brigham Programs
- Centers of Expertise
- Global & Community Health
- Health Policy & Management
- Healthcare Quality & Patient Safey
- Medical Education
- For trainees
- Prospective trainees
- Incoming trainees
- Current trainees
- Continuing Professional Development
Spider Veins vs. Varicose Veins

As you get older, your veins often become more visible beneath the surface of your skin. It’s a normal part of aging, but certain conditions can make your veins especially prominent and can even cause pain or other medical issues.
Two common vein conditions are spider veins and varicose veins. While they share some similarities, there are important differences.
“Spider veins are usually a cosmetic concern and don’t require treatment, whereas varicose veins can be more of a medical issue,” explains Sherry Scovell, MD, a vascular surgeon with the Mass General Brigham Heart and Vascular Institute. “There are lifestyle changes you can make to reduce the appearance of both, but we have medical treatments, too.”
Dr. Scovell cares for patients at Massachusetts General Hospital. She explains the difference between spider veins and varicose veins, including how they look, their causes, and treatment options.
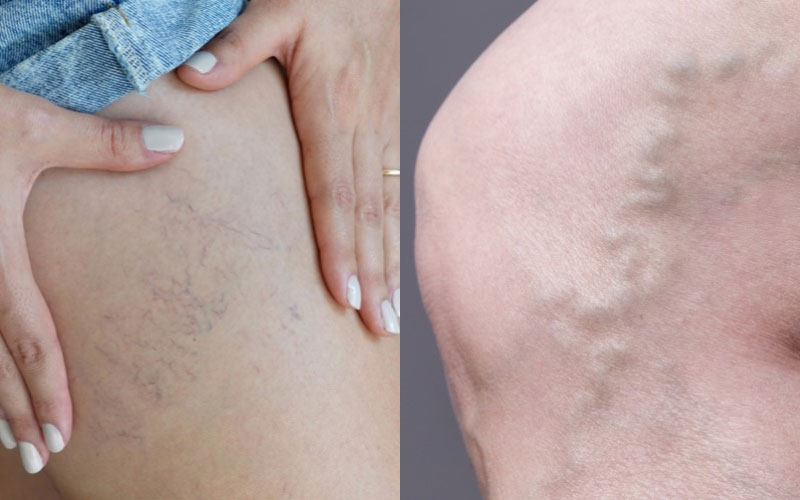
How to tell the difference between spider veins and varicose veins
Spider vein treatment
Since spider veins often don’t cause symptoms, you can make lifestyle changes to reduce their appearance and prevent new ones from forming.
However, you may choose medical treatments to treat your spider veins, or your provider may recommend it. These include:
- Sclerotherapy. A provider injects a foam or liquid into the spider vein, which creates irritation on the inside of the blood vessel and causes it to close. The reticular veins, which feed into spider veins, fade as the body absorbs them naturally. It may take a few weeks to disappear, and you may need more than one treatment. You also need to wear compression stockings for 2 weeks after the procedure.
- Laser treatments, usually for spider veins on the face or smaller spider veins where sclerotherapy isn’t an option. A provider uses a laser light to heat the blood vessels without damaging your skin. This destroys the spider vein and causes it to fade. Larger spider veins often take longer to disappear and may require additional treatment sessions.
People with spider veins may also have varicose veins. If this is the case, Dr. Scovell recommends treating the varicose veins first, as they put pressure on the smaller veins.
Varicose vein treatment
Lifestyle changes also help symptoms from varicose veins, but your provider may recommend procedures to remove them. This helps reduce symptoms, improves your blood flow, and prevents more serious complications.
Treatment for varicose veins may include:
- Sclerotherapy. This same procedure used for spider veins can also treat smaller varicose veins.
- Endovenous ablation is a common treatment for larger varicose veins. It treats superficial veins that are slightly deeper under the skin but cause the varicose veins that are visible. A physician numbs the area and inserts a flexible tube (called a catheter) into the affected vein. They close the vein by injecting a small amount of glue, chemical, or foam solution, or by using heat or laser energy. This redirects blood flow and causes the vein to close.
- Phlebectomy. This treats varicose veins that are visible under your skin and may happen at the same time as ablation. With this procedure, a physician numbs the area and makes a small poke over your varicose vein. They then use a hook-like device to remove the vein.
“Whether you have spider veins or varicose veins, talk to a provider if you’re worried about them,” Dr. Scovell recommends. “Even if you don’t have symptoms, we can help make sure you don’t have any underlying conditions and discuss possible treatments. We want you to feel comfortable in your skin.”