-
- Find Care
-
- Visitor Information
- Find a Location
- Shuttles
- Visitor Policies
-
-
- Our Virtual Care Options
- 24/7 Virtual Care
- Virtual Visits for Primary & Specialty Care
- Online Second Opinions
- Participate in Research
-
- Contact us
-
- For Innovators
- Commercialization Guide for Innovators
-
-
- Research News
- Alzheimer's Disease
- Artificial Intelligence
-
- Overview
-
- Overview
- Getting Started
- New to Mass General Brigham
- International Patient Services
- What Is Patient Gateway?
- Planning Your Visit
- Find a Doctor (opens link in new tab)
- Appointments
- Patient Resources
- Health & Wellness
- Flu, COVID-19, & RSV
- Billing & Insurance
- Financial Assistance
- Medicare and MassHealth ACOs
- Participate in Research
- Educational Resources
- Visitor Information
- Find a Location
- Shuttles
- Visitor Policies
- Find Care
-
- Overview
- Our Virtual Care Options
- 24/7 Virtual Care
- Virtual Visits for Primary & Specialty Care
- Online Second Opinions
-
- Overview
- Participate in Research
-
- Overview
- About Innovation
- About
- Team
- News
- For Industry
- Venture Capital and Investments
- World Medical Innovation Forum (opens link in new tab)
- Featured Licensing Opportunities
- For Innovators
- Commercialization Guide for Innovators
- Contact us
-
- Overview
- Information for Researchers
- Compliance Office
- Research Cores
- Clinical Trials
- Advisory Services
- Featured Research
- Two Centuries of Breakthroughs
- Advances in Motion (opens link in new tab)
- Brigham on a Mission (opens link in new tab)
- Gene and Cell Therapy Institute
- Research News
- Alzheimer's Disease
- Artificial Intelligence
-
- Overview
-
- Overview
- Residency & fellowship programs
- Brigham and Women's Hospital
- Massachusetts General Hospital
- Mass Eye and Ear
- Newton-Wellesley Hospital
- Salem Hospital
- Integrated Mass General Brigham Programs
- Centers of Expertise
- Global & Community Health
- Health Policy & Management
- Healthcare Quality & Patient Safey
- Medical Education
- For trainees
- Prospective trainees
- Incoming trainees
- Current trainees
- Continuing Professional Development
Supporting Community Needs
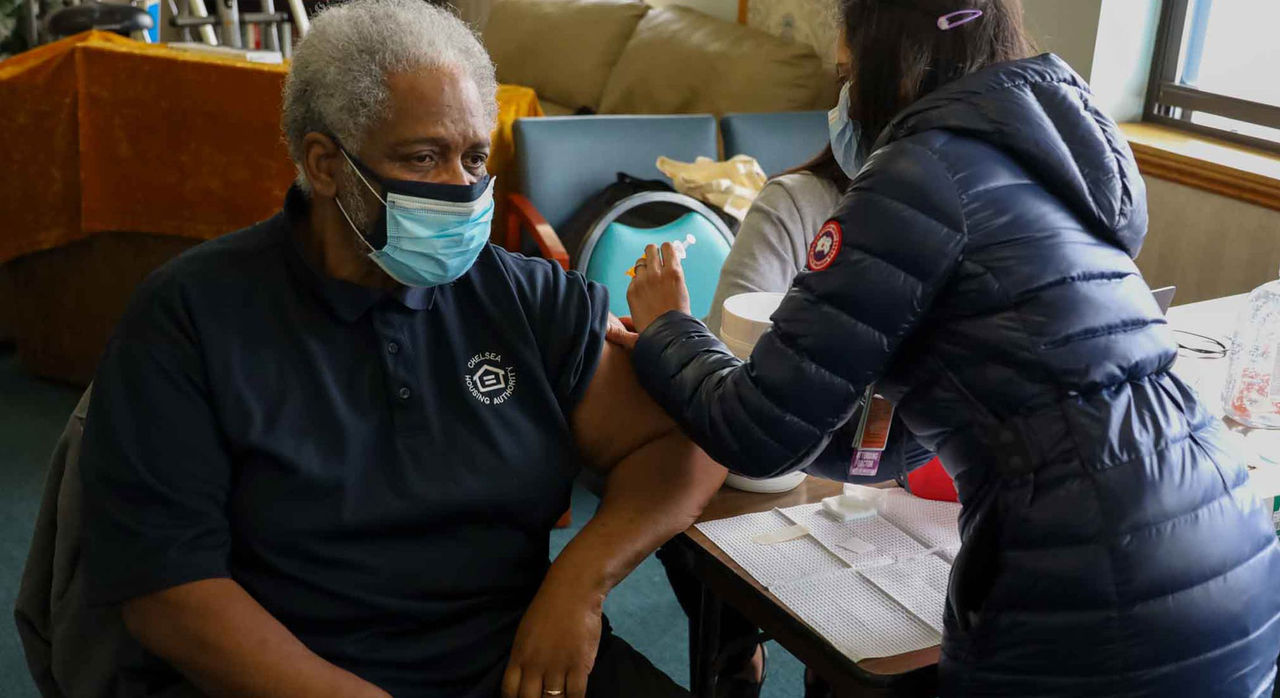
The fourth installment in a series of articles commemorating the two-year anniversary of Mass General Brigham’s United Against Racism initiative.
Systemic racism negatively influences the mental and physical health of millions of people across the United States. The impact is pervasive and deeply embedded in our society. The effects are far reaching — influencing where and how people live, learn, work, and play. These non-medical, but health-critical factors, often referred to as Social Determinants of Health (SDOH), are key drivers of health inequities within historically underserved communities, placing these populations at greater risk for poor health outcomes.
Through our United Against Racism initiative, Mass General Brigham aims to promote health equity, improve community health outcomes, and develop external advocacy programs and initiatives that support systematic changes to improve equity.
“To truly address health inequities, we need to meet people where they are, bringing health care and other supports that address social risk factors, like food insecurity, directly into the communities we serve” said Elsie Taveras, MD, MPH, Chief Community Health & Health Equity Officer at Mass General Brigham. “That means working in collaboration with community partners and listening to patients and community members to find out what is important to them.”
Engaging with Community Stakeholders
One of the most vital parts of this strategy is continued engagement with community partners. Mass General Brigham works closely with a number of non-profit organizations, community panels, and other community action groups to better understand our role in community initiatives. Feedback and evaluation help focus our services and inform the best plan of action — whether that’s financial or logistical support for existing community organizations already doing the work or standing up new Mass General Brigham programs to fill a need. One of the most intensive and formalized ways to gather this feedback is our triannual Community Needs Assessment.
A Community Needs Assessment gives organizations comprehensive information about the community's current health status, needs, and issues. This information can help develop a community health improvement plan by incorporating a comprehensive review of unmet health-related needs with a focus on the negative health impacts of social and environmental conditions. These include:
- Community input
- Analysis of public health data
- Inventory of existing programs
- Prioritization of health-related needs to be addressed
The most recent assessment helped to hone our community health strategy to focus on food security and nutrition, chronic disease management, and substance use disorders.
Food as Medicine
Access to healthy foods sits at the crossroads of social needs and healthcare. One of every five deaths across the globe is attributable to suboptimal diet, more than any other risk factor including tobacco. In the United States, fewer than 1 in 10 adolescents and adults eat enough fruits or vegetables. The impact that food has on a person’s health is increasingly referred to as “food as medicine.” It may take many forms, including medically tailored meals, access to fresh groceries, produce prescription programs, and health cooking classes.
“The recognition that what happens outside of the walls of our hospitals has a significant impact on health is essential to improving health outcomes and addressing health inequities,” says Tavinder Phull, MPH, MBA, Vice President of Community Health, Quality and Patient Experience at Mass General Brigham.
Mass General Brigham has conducted numerous research studies on the impact of nutrition on health outcomes, including how nutrition and healthy diet may influence cognitive outcomes later in life, lower risk of prostate cancer, improve response to cancer therapy, affect risk and severity of COVID-19, and reduce heartburn, among others.
This year, Mass General Brigham committed $8.4 million to promote nutrition equity and security, support food-as-medicine programs to tackle diet-related diseases, and fund food-related programming at local community-based organizations across Massachusetts. This commitment was highlighted at the White House Conference on Hunger, Nutrition, and Health by the Biden-Harris Administration, the first conference of its kind in over 50 years.
One example of this work is Mass General Brigham’s expansion of food access to patients through the MGH Revere Food Pantry. Funding will support the development of a permanent food pantry with larger storage capacity and a teaching kitchen to help showcase the power of implementing food-as-medicine programming in the community.
Mass General Brigham is also committing $6.35 million to scale effective programs and strategies at seven community-based organizations. These programs aim to reduce food insecurity, promote nutrition equity, and administer food-as-medicine programs and medically tailored meals in Massachusetts. One of these community partnerships, The Phoenix Food hub, recently opened in Lynn to offer residents a wide range of nutritional and service support including a teaching kitchen, food distribution, counseling for SNAP and WIC, among many other resources.
Meeting People Where They Are
Over the course of the pandemic, many people have delayed their medical care. Chronic disease management, for example, has declined tremendously, leading to sicker patients. As a healthcare organization, Mass General Brigham looks for ways to connect with members of local communities that are most difficult to reach and who are often disproportionately affected by adverse outcomes. Our Community Care Van program can engage hard-to-reach populations in a more effective, equitable way.
This “clinic on wheels” offers screenings and interventions for chronic health issues such as hypertension, diabetes, and substance use disorders, in addition to COVID-19 screening and vaccinations. The vans are staffed with multilingual and multicultural clinicians and support staff to better connect with the communities served by Mass General Brigham.
The van program was initially launched in 2021 to support areas hardest hit by the COVID-19 pandemic. At the outset, the program’s goal was to provide COVID testing, vaccines, and reliable health information to thousands of people. Two recently published papers from Mass General Brigham demonstrate the effectiveness of bringing COVID-19 health care services to where people need them the most. The vans’ schedule is routinely updated with stops in Lynn, Chelsea, Revere, Everett, and Greater Boston — including Charlestown, Dorchester, Roxbury, Mattapan, and Jamaica Plain.
Staff on the vans also screen visitors for critical non-medical health factors. These SDOH screenings ask patients about issues such as housing, access to healthy food, and personal safety. Connecting patients with appropriate resources can have a far-reaching impact on a variety of health concerns.
As COVID becomes more ingrained in our day-to-day lives, the vans are evolving to meet more diverse needs. The expanded services on the vans identify target interventions for specific, widescale problems starting with hypertension and diabetes care. Clinicians can screen blood pressure, test for lipid and A1C levels, and provide physical activity assessments. Staff can also provide recommendations for additional physician follow-ups and a blood pressure care plan.
In 2023, the mobile vans will add substance use disorder (SUDs) services to their rotation. Clinicians on the van will provide initial screenings, make connections for patients to treatment programs and recovery coaching, and provide prescription-based treatment options.
This is just a small sample of all the incredible work happening across the system to support community health. For a deeper dive into this strategy, we recommend reading our interview with Tavinder Phull, MPH, MBA, Vice President of Community Health and Health Equity.
In our next installment, Tom Sequist, Chief Medical Officer at Mass General Brigham, reflects on the past year of United Against Racism initiatives and what he’s excited about for the coming year.
If you missed it, read our previous article, “Bridging the Digital Divide” along with our interview with Dr. Lee Park, Chief Patient Experience Officer at Mass General Brigham.