-
- Find Care
-
- Visitor Information
- Find a Location
- Shuttles
- Visitor Policies
-
-
- Our Virtual Care Options
- 24/7 Virtual Care
- Virtual Visits for Primary & Specialty Care
- Online Second Opinions
- Participate in Research
-
- Contact us
-
- For Innovators
- Commercialization Guide for Innovators
-
-
- Research News
- Alzheimer's Disease
- Artificial Intelligence
-
- Overview
-
- Overview
- Getting Started
- New to Mass General Brigham
- International Patient Services
- What Is Patient Gateway?
- Planning Your Visit
- Find a Doctor (opens link in new tab)
- Appointments
- Patient Resources
- Health & Wellness
- Flu, COVID-19, & RSV
- Billing & Insurance
- Financial Assistance
- Medicare and MassHealth ACOs
- Participate in Research
- Educational Resources
- Visitor Information
- Find a Location
- Shuttles
- Visitor Policies
- Find Care
-
- Overview
- Our Virtual Care Options
- 24/7 Virtual Care
- Virtual Visits for Primary & Specialty Care
- Online Second Opinions
-
- Overview
- Participate in Research
-
- Overview
- About Innovation
- About
- Team
- News
- For Industry
- Venture Capital and Investments
- World Medical Innovation Forum (opens link in new tab)
- Featured Licensing Opportunities
- For Innovators
- Commercialization Guide for Innovators
- Contact us
-
- Overview
- Information for Researchers
- Compliance Office
- Research Cores
- Clinical Trials
- Advisory Services
- Featured Research
- Two Centuries of Breakthroughs
- Advances in Motion (opens link in new tab)
- Brigham on a Mission (opens link in new tab)
- Gene and Cell Therapy Institute
- Research News
- Alzheimer's Disease
- Artificial Intelligence
-
- Overview
-
- Overview
- Residency & fellowship programs
- Brigham and Women's Hospital
- Massachusetts General Hospital
- Mass Eye and Ear
- Newton-Wellesley Hospital
- Salem Hospital
- Integrated Mass General Brigham Programs
- Centers of Expertise
- Global & Community Health
- Health Policy & Management
- Healthcare Quality & Patient Safey
- Medical Education
- For trainees
- Prospective trainees
- Incoming trainees
- Current trainees
- Continuing Professional Development
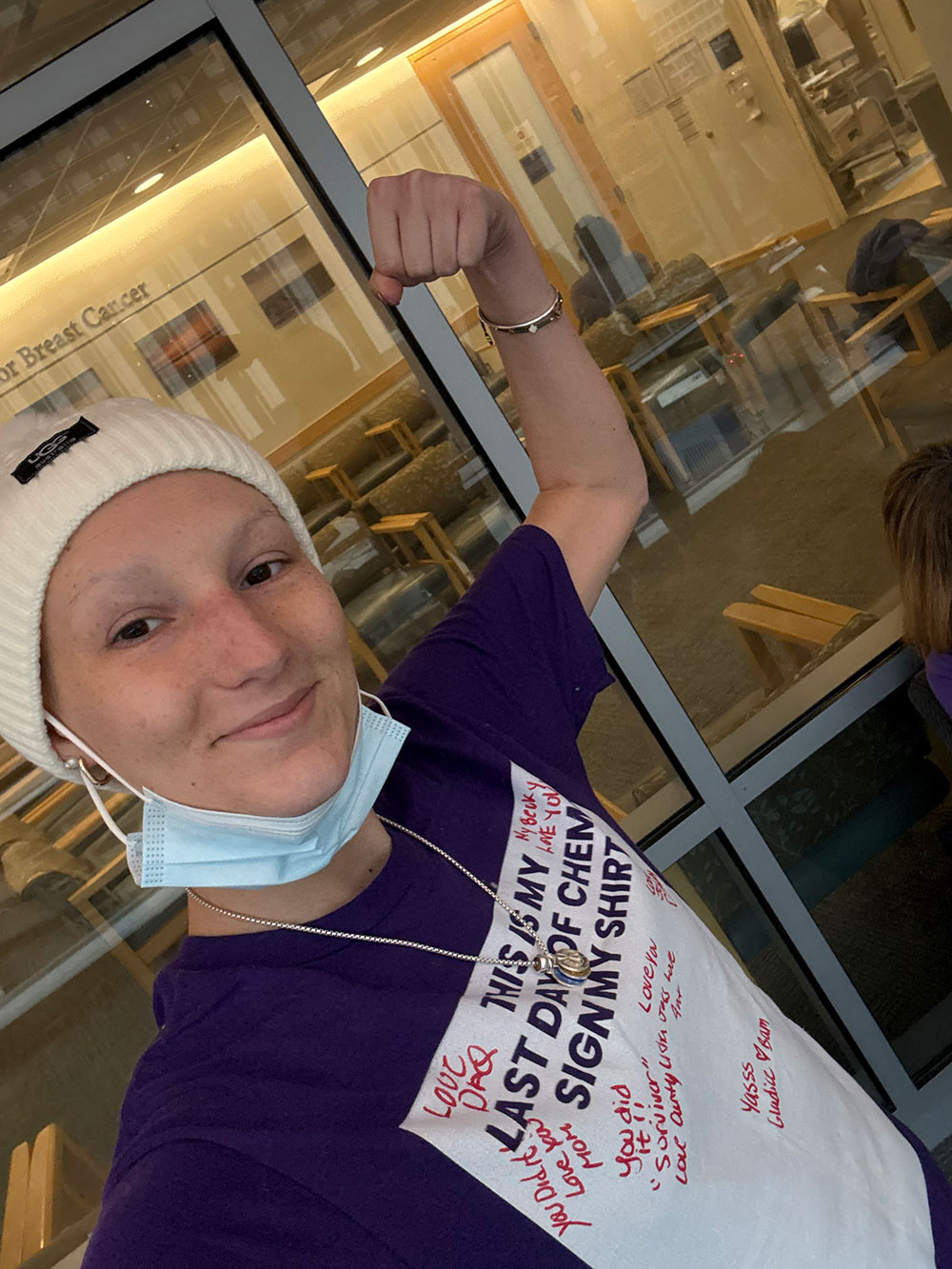
Highly Specialized, Integrated Care Takes Young Lymphoma Patient from Rare Diagnosis to Cure
When Jessica Holmes, 25, kept getting bouts of strep throat last January, she didn’t give it much thought at first. As a paraprofessional in the Quincy Public Schools, “I do work with children,” she acknowledged.
Still, it was a lot. And she was otherwise healthy and active. In fact, she was in peak physical condition, having just achieved a personal best at the gym — deadlifting 215 lbs. at a bodyweight of 125 lbs. She was also quite busy. In between work, family and friends, she was pursuing a master’s degree in psychology.
How serious could a few sore throats be? Maybe she just needed to slow down, she thought.
“Then I started getting lumps on my neck, and I’d never had that before,” Jessica said. “My body was trying to tell me something.”
She listened to it — a decision that would upend her life but also save it. As Jessica would soon learn, she had Hodgkin lymphoma, a rare form of lymph node cancer that primarily affects young people.
And thanks to the world-class, multidisciplinary care she received at Mass General Brigham Cancer Institute, Jessica is now cancer-free and gradually returning to her normal — and delightfully busy — life.