Mass General Brigham Investigators Identify New Genetic Variant Protective Against Alzheimer’s Disease
- Working with an international team, researchers identified a new patient with a genetic predisposition for early-onset Alzheimer’s disease who remained cognitively intact more than two decades beyond the expected age of memory impairment
- The case has led to the discovery of a protective variant, a pathway for ‘resilience’ to dementia, and the identification of a brain region to target with therapeutics
A single patient can spark new research questions and provide answers about a disease. And when a new case is identified, investigators can make connections between them that can lead to even more powerful and persuasive ideas about cause and treatment. In a publication today in Nature Medicine, an international team led by investigators from two Mass General Brigham hospitals — Massachusetts General Hospital (MGH) and Mass Eye and Ear — reports on a new case of a patient with a genetic predisposition for developing early-onset Alzheimer’s disease who remained cognitively intact until his late 60s. Through clinical assessments led by investigators at the University of Antioquia in Colombia, genetic and molecular studies performed at Mass Eye and Ear, and Children’s Hospital Los Angeles, neuroimaging and biomarker studies conducted at MGH, and neuropathological studies carried out by investigators at University Medical Center Hamburg-Eppendorf in Germany, the team identified a new genetic variant that provides protection from Alzheimer’s disease. The variant occurs in a different gene than in a case from the same family reported in 2019 but points to a common disease pathway. Insights from their findings also pinpoint a region of the brain that may provide an optimal treatment target in the future.
“The genetic variant we have identified points to a pathway that can produce extreme resilience and protection against Alzheimer’s disease symptoms,” said co-senior author Joseph F. Arboleda-Velasquez, MD, PhD, an associate scientist at Mass Eye and Ear. “These are the kinds of insights we cannot gain without patients. They are showing us what’s important when it comes to protection and challenging many of the field’s assumptions about Alzheimer’s disease and its progression.”
The case that caught the investigators’ attention involved a family member of the world’s largest-known kindred with a genetic variant called the “Paisa” mutation (Presenilin-1 E280A). Carriers of this variant usually develop mild cognitive impairment at a median age of 44, dementia at age 49, and die from complications of dementia in their 60s. Francisco Lopera, MD, director of the Neuroscience Group of Antioquia in Medellín, Colombia, a co-first author of the Nature Medicine paper, is the neurologist who discovered this family and has been following them for the last 30 years. This team of investigators previously studied a woman from this family who remained unimpaired until her 70s and whose case was reported in 2019. In their new Nature Medicine paper, the investigators describe a case of a male carrier of the Paisa mutation who remained cognitively intact until age 67. He progressed to mild dementia at age 72 and died at 74 — decades after most people with the Paisa mutation typically do.
“Extraordinary cases like this one illustrate how individuals and extended families with Alzheimer’s disease can help advance our understanding of the disease and open new avenues for discovery,” said co-senior author Yakeel T. Quiroz, PhD, a clinical neuropsychologist and neuroimaging researcher, director of the Familial Dementia Neuroimaging Lab in the Departments of Psychiatry and Neurology at Massachusetts General Hospital. “The insights we are gaining from this second case may guide us on where in the brain we need to look to delay and stop disease progression and will help us form new hypotheses about the series of steps that may actually lead to Alzheimer’s dementia.”
“What we have done with the study of these two protected cases is to read mother nature,” said Lopera. “The most exciting thing is that nature has revealed to us both the cause of Alzheimer’s and the cure for it. Mother nature did an exceptional experiment with these two subjects: it endowed them both with a gene that causes Alzheimer's and at the same time with another gene that protected them from the symptoms of the disease for more than two decades. Therefore, the solution is to imitate nature by developing therapies that mimic the mechanism of protection of these genetic variants in subjects at risk of suffering from the disease.”
Lopera added, “A great door has been opened for the prevention and treatment of incurable diseases.”
The male patient was enrolled in the Mass General Colombia-Boston biomarker study (COLBOS), which brings members of an extended family group of 6,000 individuals with the known Paisa mutation to Boston for advanced neuroimaging, biomarker and genetic examinations. The same study previously detected a case in which a female patient carried two copies of a rare Christchurch genetic variant, which affects APOE3 — a protein that is heavily implicated in Alzheimer’s disease. However, the researchers ruled out the presence of the APOE Christchurch genetic variant in the male patient. The team performed genetic and molecular analyses at Mass Eye and Ear in collaboration with Xiaowu Gai Ph.D. and colleagues from Children’s Hospital Los Angeles to identify other variants that could have been protecting him from Alzheimer’s disease. The most promising candidate was a new and rare variant, never before reported in the Reelin gene. The team named it Reelin-COLBOS. In studies led by co-senior author Diego Sepulveda-Falla, MD, a principal investigator at the Institute of Neuropathology at the University Medical Center Hamburg-Eppendorf, the team further verified the protective role of the Reelin-COLBOS variant in mouse models and neuropathological studies.
“Each of the protected cases, the APOE Christchurch and the Reelin-COLBOS case, shows a distinctive protective pattern in the postmortem analyses, one global and the other very localized,” said Sepulveda-Falla. “These outstanding cases are teaching us that Alzheimer’s protection can take different shapes, and that perhaps a therapy can be successful just by targeting key brain structures such as the entorhinal cortex. They are forcing us to revise our previous concepts about neurodegeneration and cognitive decline. These are exciting times for us, and hopefully for the Alzheimer’s research field as well.”
The researchers describe Reelin as a “cousin” of the more famous APOE. Both Reelin and APOE compete to bind to similar cellular receptors, essentially jostling to occupy the same seat. When Reelin sits in the receptor seat, it diminishes the phosphorylation of tau, a protein known to form pathological tangles in brains with Alzheimer’s disease. When APOE binds the receptor, it has the opposite effect.
Reelin is a protein with a pivotal role in the regulation of brain cell development and function. In fact, previous reports have linked mutations in Reelin to diseases like autism, schizophrenia, epilepsy, and bipolar disorder. However, mutations linked to disease are different because they diminish the protein’s function, whereas, in the case of Reelin-COLBOS, the protective variant increases the function of the protein.
“When we saw that one of our top candidates for the variant sat in Reelin, it was a bit shocking,” said Arboleda-Velasquez. “The fact that the first case showed us a variant affecting APOE and the second case affects Reelin tells us that this signaling pathway that controls the phosphorylation of tau, among other effects, may be key to understanding why these patients were protected. This is critical to guide therapies because it clearly tells us that more Reelin could potentially have beneficial effects.”
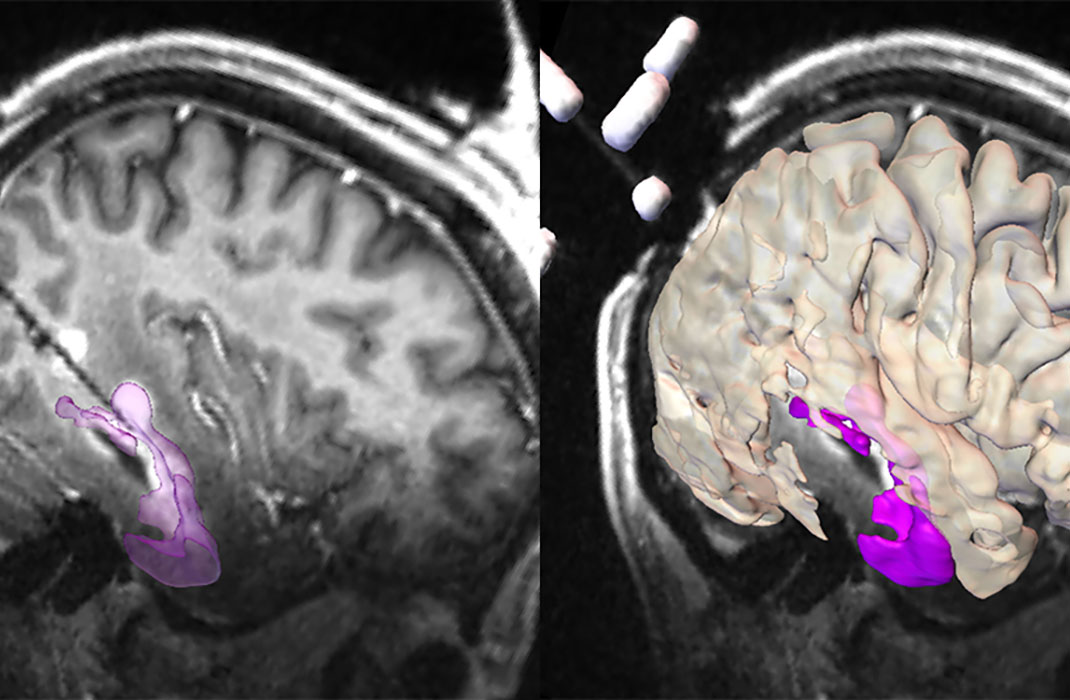
The most recent patient underwent neuroimaging exams at Massachusetts General Hospital at age 73. These scans revealed that while the patient’s amyloid-beta plaque burden was high and he had tau tangles in some regions of his brain, his entorhinal cortex had notably very limited tau pathology. The entorhinal cortex plays a critical role in memory and learning, and its degeneration is known to lead to cognitive impairment and dementia. Studies in a mouse model also showed that the Reelin-COLBOS variant protected against tau pathology.
“This case indicates that the entorhinal region may represent a tiny target that’s critical for protection against dementia,” said Quiroz.
As investigators pursue gene therapies that may in the future deliver treatments that can modify or manipulate gene expression, understanding what region of the brain to focus on for delivery will become increasingly important.
Many treatments for Alzheimer’s disease, including drugs recently approved by the U.S. Food and Drug Administration and other drugs currently in clinical trials, target reducing amyloid plaque buildup. The study’s results point to potential new avenues for treatment because the two patients with protection had extremely high levels of amyloid in their brains and yet they were protected.
“These exciting findings demonstrate the power of academic collaboration, where a retinal disease genetics expert working with a local neuroimaging authority can team up with leading neurologists and neuropathologists around the world to power scientific discovery,” said Joan W. Miller, MD, chair of Ophthalmology at Mass Eye and Ear, Mass General Hospital and Brigham and Women’s Hospital, and David Glendenning Cogan Professor and chair of Ophthalmology at Harvard Medical School. “Alzheimer’s disease remains a devastating disease with an immense global burden, and this work opens the door to further investigation into how this resilience pathway may lead to an effective therapeutic strategy.”
The researchers note that they cannot completely rule out that other factors, including additional gene variants, may have contributed to the patient’s resilience against Alzheimer’s disease symptoms. But their experimental evidence in preclinical studies strongly implicate the Reelin-COLBOS variant.
Arboleda-Velasquez and Quiroz, together with Lopera and Sepulveda-Falla, plan to continue their work to identify additional protected patients from these Colombian families, learning from each extraordinary case. They are also conducting research looking at treatments to target this protective pathway.
“It is a huge privilege to have these genetic cases to work on,” said Arboleda-Velasquez. “We are honored to be a part of the team that has made this discovery.”
Authorship: Co-first authors of this publication are: Francisco Lopera, Claudia Marino, Anita S. Chandrahas, Michael O’Hare and Nelson David Villalba-Moreno.
Disclosures: Arboleda-Velasquez and co-author Leo A. Kim M.D., Ph.D. are co-founders of Epoch Biotech, LLC, a biotech developing resilient case-inspired therapeutics. Quiroz and Lopera serve as consultants for Biogen.
Funding: This work was supported primarily through philanthropy to Mass Eye and Ear, including Open Philanthropy and Good Ventures, and the Remondi Family Foundation. The work was supported by National Institutes of Health (DP5 OD019833), National Institute on Aging (R01 AG054671), the Massachusetts General Hospital Executive Committee on Research (MGH Research Scholar Award), the Alzheimer’s Association, the National Institute of Neurological Disorders and Stroke (UH3 NS100121 and RF1 NS110048), the German Federal Ministry of Education and Research, UndoAD Project, the German Research Foundation (SFB877), and the API Colombia.
Paper cited: Lopera F et al. “Resilience to autosomal dominant Alzheimer’s disease in a Reelin-COLBOS heterozygous man” Nature Medicine DOI: https://doi.org/10.1038/s41591-023-02318-3
Contact
About Mass General Brigham
Mass General Brigham is an integrated academic health care system, uniting great minds to solve the hardest problems in medicine for our communities and the world. Mass General Brigham connects a full continuum of care across a system of academic medical centers, community and specialty hospitals, a health insurance plan, physician networks, community health centers, home care, and long-term care services. Mass General Brigham is a nonprofit organization committed to patient care, research, teaching, and service to the community. In addition, Mass General Brigham is one of the nation’s leading biomedical research organizations with several Harvard Medical School teaching hospitals. For more information, please visit massgeneralbrigham.org.
Related research about Alzheimer’s disease
-

published on
-

published on
-

published on
-
published on
-

published on
-

published on
-

published on
-

published on
-

published on