-
- Find Care
-
- Visitor Information
- Find a Location
- Shuttles
- Visitor Policies
-
-
- Our Virtual Care Options
- 24/7 Virtual Care
- Virtual Visits for Primary & Specialty Care
- Online Second Opinions
- Participate in Research
-
- Contact us
-
- For Innovators
- Commercialization Guide for Innovators
-
-
- Research News
- Alzheimer's Disease
- Artificial Intelligence
-
- Overview
-
- Overview
- Getting Started
- New to Mass General Brigham
- International Patient Services
- What Is Patient Gateway?
- Planning Your Visit
- Find a Doctor (opens link in new tab)
- Appointments
- Patient Resources
- Health & Wellness
- Flu, COVID-19, & RSV
- Billing & Insurance
- Financial Assistance
- Medicare and MassHealth ACOs
- Participate in Research
- Educational Resources
- Visitor Information
- Find a Location
- Shuttles
- Visitor Policies
- Find Care
-
- Overview
- Our Virtual Care Options
- 24/7 Virtual Care
- Virtual Visits for Primary & Specialty Care
- Online Second Opinions
-
- Overview
- Participate in Research
-
- Overview
- About Innovation
- About
- Team
- News
- For Industry
- Venture Capital and Investments
- World Medical Innovation Forum (opens link in new tab)
- Featured Licensing Opportunities
- For Innovators
- Commercialization Guide for Innovators
- Contact us
-
- Overview
- Information for Researchers
- Compliance Office
- Research Cores
- Clinical Trials
- Advisory Services
- Featured Research
- Two Centuries of Breakthroughs
- Advances in Motion (opens link in new tab)
- Brigham on a Mission (opens link in new tab)
- Gene and Cell Therapy Institute
- Research News
- Alzheimer's Disease
- Artificial Intelligence
-
- Overview
-
- Overview
- Residency & fellowship programs
- Brigham and Women's Hospital
- Massachusetts General Hospital
- Mass Eye and Ear
- Newton-Wellesley Hospital
- Salem Hospital
- Integrated Mass General Brigham Programs
- Centers of Expertise
- Global & Community Health
- Health Policy & Management
- Healthcare Quality & Patient Safey
- Medical Education
- For trainees
- Prospective trainees
- Incoming trainees
- Current trainees
- Continuing Professional Development
Lyme Disease in Kids: Signs, Symptoms, Treatment, and Prevention

When the snow finally melts and spring arrives, kids and parents alike are eager to get outside. But in the back of many parents’ minds lurks a common worry: Lyme disease.
Lyme disease is a bacterial infection spread by tick bites. It’s worth paying attention to — especially since cases have been rising over the last decade or so. But that doesn’t mean you need to forego time in the great outdoors, explains Daniel A. Solomon, MD, a Mass General Brigham infectious diseases doctor who cares for patients at Brigham and Women’s Hospital.
“It’s important to be attuned to symptoms that could be early signs of Lyme disease. It’s easiest to treat when it’s identified early,” Dr. Solomon says. “And there are a lot of things you can do to decrease the risk for you and your family.”
Who is at risk for Lyme disease?
Lyme disease cases have been reported all over the U.S. But it’s most common in the Northeast and the upper Midwest area of Wisconsin and Minnesota. “Those are the hot spots where we see by far the most cases,” Dr. Solomon says.
Lyme disease risk is greatest during late spring and early summer, when ticks are most active. It can affect people of all ages who spend time outside. The disease is spread by black-legged ticks, which spend their lives low to the ground in grasses and shrubs. “The biggest risk comes from being outside in grassy areas or wooded areas with low bushes,” Dr. Solomon says.
Lyme disease prevention
The best way to protect your kids (and yourself) from Lyme disease is to prevent tick bites in the first place. These strategies can help:
Wear long pants and socks when you’re in areas with low shrubs and long grasses.
Wear light-colored clothing. Ticks are black, so they’re easier to spot against a lighter colored background.
Treat clothes and shoes with permethrin, a chemical that repels ticks. The insecticide is safe for kids but isn’t designed for use on skin. Instead, it should be sprayed on clothing to keep ticks at bay.
Use bug spray containing DEET to help ward off ticks. Insect repellants with no more than 30% DEET are safe for kids older than 2 months. But it can be toxic if swallowed, so don’t let younger kids spray themselves. When spraying DEET on children, avoid getting it on their hands or near their eyes and mouth.
Put clothes in the dryer on high heat for 10 minutes after you come inside. “That will kill any ticks that are crawling on the clothes,” Dr. Solomon says.
Shower to wash off any ticks that haven’t attached yet. Then do a thorough tick check afterward. They like to hide in dark crevices, so check out-of-the-way spots like the underarms, behind the knees, behind ears, inside the belly button, and in the groin.
I found a tick. Now what?
Ticks attach to the skin with their mouthparts, and can stay attached for many hours. To remove one, use tweezers to grab the tick as close to the skin as possible and pull straight up. Sometimes, little bits of mouthparts are left in the skin. “Don’t dig them out, because you could cause an infection,” Dr. Solomon says. They will work their way out on their own.
The good news: It takes time for the Lyme disease bacterium to move from the tick into a person’s blood. If you know the tick was attached for less than 36 hours, it probably didn’t have time to spread the disease.
If you live in an area where Lyme disease is common, and aren’t sure how long the tick was attached, Dr. Solomon recommends taking action to prevent getting sick. You can ask your doctor for “post-exposure prophylaxis” — a single dose of the antibiotic doxycycline. “That single-dose treatment is very effective at decreasing the risk of Lyme disease,” he says. “It’s safe for kids and adults, but you need to take it within 72 hours of the tick bite, and ideally as soon as possible.”
Lyme disease symptoms
Ticks are tiny, and sometimes bites go under the radar. So it’s important to be on the lookout for signs of Lyme disease in kids, Dr. Solomon says.
Symptoms of early Lyme disease
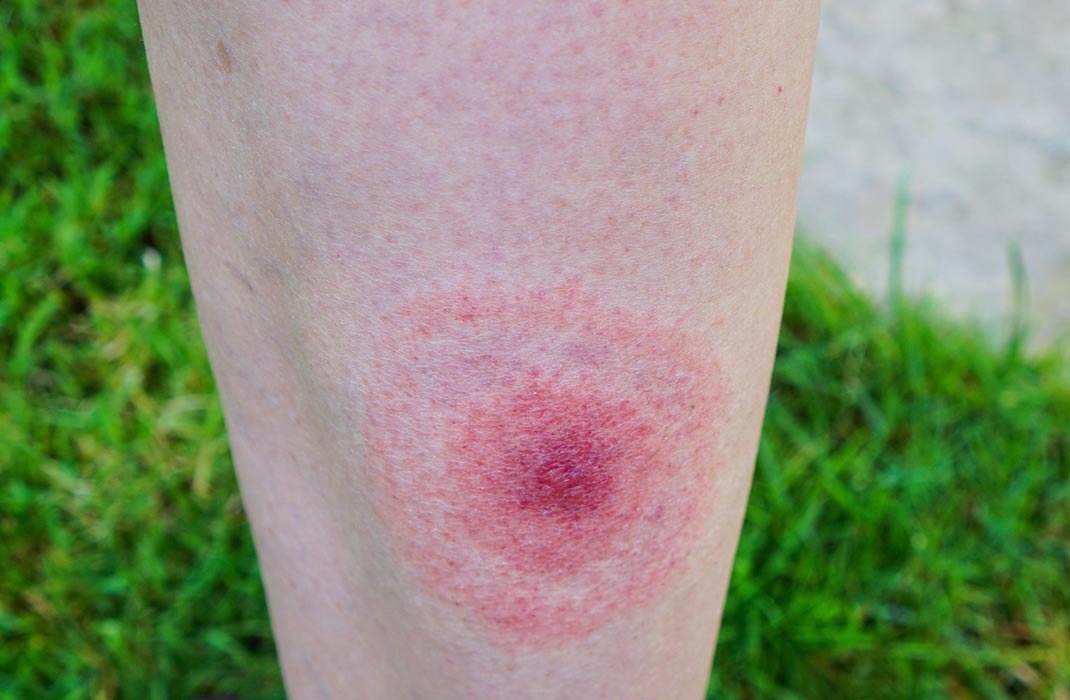
For many people, a rash is the only symptom of early Lyme disease. But about a third of people have symptoms that extend beyond the skin:
- Low-grade fever
- Muscle aches
- Fatigue
“If you have what seems like a summer flu, it could be early-stage Lyme disease,” Dr. Solomon says.
Symptoms of later-stage Lyme disease
If Lyme disease isn’t diagnosed and treated early, it can spread through the body, advancing to Stage 2 Lyme disease. Symptoms of Stage 2 typically show up 3 to 10 weeks after the tick bite.
Symptoms can include:
- Heart rhythm problems
- Bell’s palsy (weakness or paralysis on one side of the face)
- Numbness or pain
If it continues untreated, that can advance to Stage 3 Lyme, with symptoms such as:
- Arthritis (stiff, swollen joints)
- Muscle weakness or twitching
- Speech problems
- Cognitive problems (difficulty with thinking and memory)
Lyme disease diagnosis
The rash is the best way to identify early-stage Lyme disease, Dr. Solomon says. Blood tests for Lyme disease are available, but they aren’t very good at picking up the earliest stages of the disease. For that reason, you should get treatment right away if you have a Lyme rash—even if you have a negative blood test.
After 2 to 6 weeks, your body will start producing antibodies against Lyme disease. At that point, blood tests can detect the antibodies. The blood test is done in two stages. If the first step comes back positive for Lyme, the laboratory will perform a second test to confirm the diagnosis. During Stage 2 and 3 Lyme disease, the blood test successfully identifies the disease in 9 out of 10 people, Dr. Solomon says.
If you remove a tick, it’s possible to send it off to be tested for Lyme disease, he adds. But he doesn’t usually recommend it. “If we know a patient had a tick bite, I want to start the single-dose antibiotic to prevent Lyme disease,” he says. “We want to give that as quickly as possible, so it doesn’t pay to wait for the results of a tick test.”
Lyme disease treatment
Lyme disease is treated with a course of antibiotics. If you or your child has a rash or other early signs, the doctor will probably prescribe the drugs for 10 to 14 days.
If you have Stage 2 or 3 Lyme disease, you may need to take the medication longer, depending on how serious the symptoms are.
For most people, antibiotic treatment squashes the infection, and symptoms go away. Some people, though, develop what’s known as post-treatment Lyme disease. They may continue to have problems such as low energy, brain fog, and difficulty concentrating. “This is a real syndrome, but it doesn’t seem to be caused by continued infection,” Dr. Solomon says. Instead, experts suspect the infection sets off a reaction in the body’s immune system and nervous system, which causes lingering symptoms.
Unfortunately, studies have shown that long-term use of antibiotics doesn’t help improve post-treatment Lyme disease. Many of the symptoms are similar to other illnesses, including long COVID. If you experience these signs, see your doctor to rule out other problems and help you find ways to manage the symptoms.
Other tick-borne diseases
One more word of caution before you head outside: Lyme disease isn’t the only infection caused by tricky ticks. “There are other tick-borne infections you should be aware of,” Dr. Solomon says. In the Northeast, anaplasmosis and babesiosis are common. In the Midwest, ehrlichiosis is another possible illness spread by ticks.
These diseases cause similar symptoms to Lyme disease, including fever, chills, and muscle aches. They can also be treated with antibiotics—but some require a different type of antibiotics. “If you’re treated for Lyme disease but still have symptoms, ask your doctor if you should consider treatment for one of these other diseases,” Dr. Solomon says.
Reading about Lyme disease and the other tick-borne illnesses can feel overwhelming. Ticks aren’t something to take lightly. But by taking steps to avoid tick bites and treat symptoms early, you can keep the crawly critters from derailing your summer fun.