-
- Find Care
-
- Visitor Information
- Find a Location
- Shuttles
- Visitor Policies
-
-
- Our Virtual Care Options
- 24/7 Virtual Care
- Virtual Visits for Primary & Specialty Care
- Online Second Opinions
- Participate in Research
-
- Contact us
-
- For Innovators
- Commercialization Guide for Innovators
-
-
- Research News
- Alzheimer's Disease
- Artificial Intelligence
-
- Overview
-
- Overview
- Getting Started
- New to Mass General Brigham
- International Patient Services
- What Is Patient Gateway?
- Planning Your Visit
- Find a Doctor (opens link in new tab)
- Appointments
- Patient Resources
- Health & Wellness
- Flu, COVID-19, & RSV
- Billing & Insurance
- Financial Assistance
- Medicare and MassHealth ACOs
- Participate in Research
- Educational Resources
- Visitor Information
- Find a Location
- Shuttles
- Visitor Policies
- Find Care
-
- Overview
- Our Virtual Care Options
- 24/7 Virtual Care
- Virtual Visits for Primary & Specialty Care
- Online Second Opinions
-
- Overview
- Participate in Research
-
- Overview
- About Innovation
- About
- Team
- News
- For Industry
- Venture Capital and Investments
- World Medical Innovation Forum (opens link in new tab)
- Featured Licensing Opportunities
- For Innovators
- Commercialization Guide for Innovators
- Contact us
-
- Overview
- Information for Researchers
- Compliance Office
- Research Cores
- Clinical Trials
- Advisory Services
- Featured Research
- Two Centuries of Breakthroughs
- Advances in Motion (opens link in new tab)
- Brigham on a Mission (opens link in new tab)
- Gene and Cell Therapy Institute
- Research News
- Alzheimer's Disease
- Artificial Intelligence
-
- Overview
-
- Overview
- Residency & fellowship programs
- Brigham and Women's Hospital
- Massachusetts General Hospital
- Mass Eye and Ear
- Newton-Wellesley Hospital
- Salem Hospital
- Integrated Mass General Brigham Programs
- Centers of Expertise
- Global & Community Health
- Health Policy & Management
- Healthcare Quality & Patient Safey
- Medical Education
- For trainees
- Prospective trainees
- Incoming trainees
- Current trainees
- Continuing Professional Development
Urgent Care for Rashes

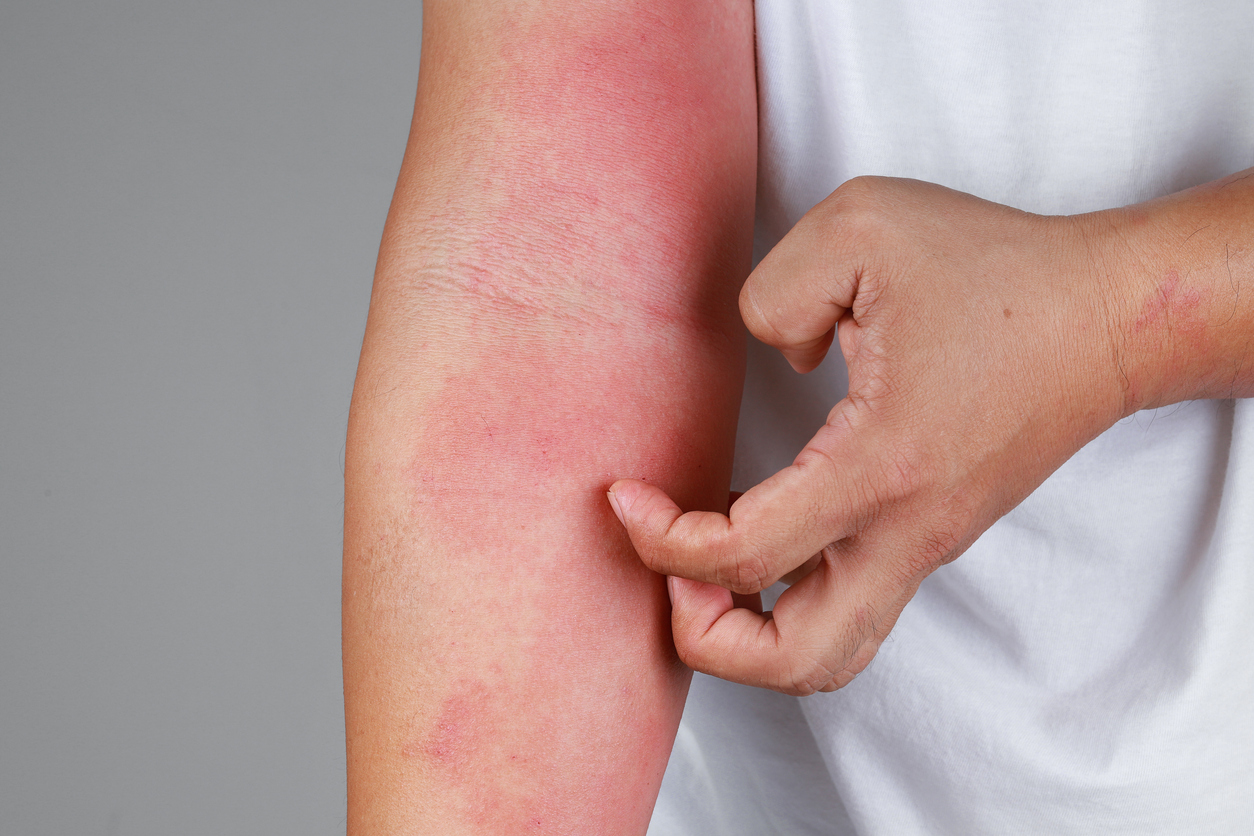
Rashes—areas of bumpy, irritated, or swollen skin—are incredibly common and can be extremely uncomfortable. You’ve probably had one at some point in your life, whether you’ve stepped in poison ivy or had a reaction to a new body wash.
“Rashes are such a broad category, and can range from something that resolves after a couple of hours to having a cause that can be extremely dangerous, and everything in between,” says Mass General Brigham emergency medicine doctor Joseph W. Kopp, MD. In this article, learn more about the different types of rashes and when you should seek medical attention.
When should you seek medical care for a rash?
If you or a family member has a new rash, call your primary care provider (PCP). Your doctor's office can recommend next steps and assist with any urgent issues.
“It’s always a good idea to contact your PCP first. They know you the best, they know your medical and family history, and they can tease out some of those subtle details,” explains Dr. Kopp.
It’s especially important to call your PCP if you have any of these signs or symptoms, which may indicate a more serious medical problem:
- A fever
- Feeling dizzy or lightheaded
- A racing heart rate
- A rash that has spread to your mucus membranes (the lining of the nose or mouth)
- A rash along your groin, your joints, or the palms of your hands
- A rash with blistering or bleeding
If you’re having trouble breathing, or you’ve had a previous episode of a serious allergic reaction known as anaphylaxis, call 911 or go to the emergency room.
If you have a rash that’s not a medical emergency, many Mass General Brigham primary care practices for adults and children offer same-day, in-person, and virtual visits. If you don’t have a PCP or no appointments are available, you can go to urgent care.
How do health care providers diagnose a skin rash?
During an in-person visit for a rash, health care providers examine your skin carefully, touching the surface of the rash. They take vital signs, like your temperature, and may order blood work. Your provider will ask questions about your lifestyle, diet, and things you may have come in contact with that may be causing the rash.
Dr. Kopp recommends that patients take photos to keep a visual record of their rash. “If you’re being seen after you’ve had the rash for a couple of days, it can be really helpful to have pictures to show how the rash might have changed,” he says.
Seeing how your rash has evolved over time will help your health care provider diagnose and treat it. When it comes to diagnosing and treating rashes, it’s important that patients can identify anything new or unusual when it comes to their skin.
Rashes in patients with darker skin tones
“For people with darker skin, it can be much more difficult to see rashes in detail,” Dr. Kopp advises. “That’s when the patient’s input will be very important.”
“We teach our residents and our med students to pay more attention and ask the detailed questions so that we’re not missing any of those dangerous rashes in our patients with darker skin tones,” says Dr. Kopp. This approach to medical education is one way that Mass General Brigham is committed to making clinical care more equitable.
Can I see a virtual doctor for a rash?
For most rashes, seeing a health care provider in person is best so they can examine and touch the rash. “There are important medical differences between a rash that’s flat, that you can’t feel, versus a rash that has bumps on the surface or is textured, which can lead you in a different direction in terms of the cause,” says Dr. Kopp.
For mild rashes, Mass General Brigham 24/7 Virtual Care is also an option for care. It’s open to all patients ages 3 and up, even if they haven’t seen a Mass General Brigham provider before. Both new and current patients can schedule a 24/7 Virtual Care visit for that day or the next day on Mass General Brigham Patient Gateway.
“It will be a more limited exam of the skin using a camera. We won’t be able to examine any sensitive areas, like the groin. But we can do an initial evaluation and recommend if patients need to get any additional testing or should be seen in person,” Dr. Kopp says.
Common causes of skin rashes
Rashes have a wide range of causes, including:
- Infection
- Allergens or irritants
- Bug bites
- Autoimmune diseases
Infection
Rashes can stem from viruses, bacteria, fungi, or parasites that cause infections like:
- Shingles
- Cellulitis
- Chickenpox
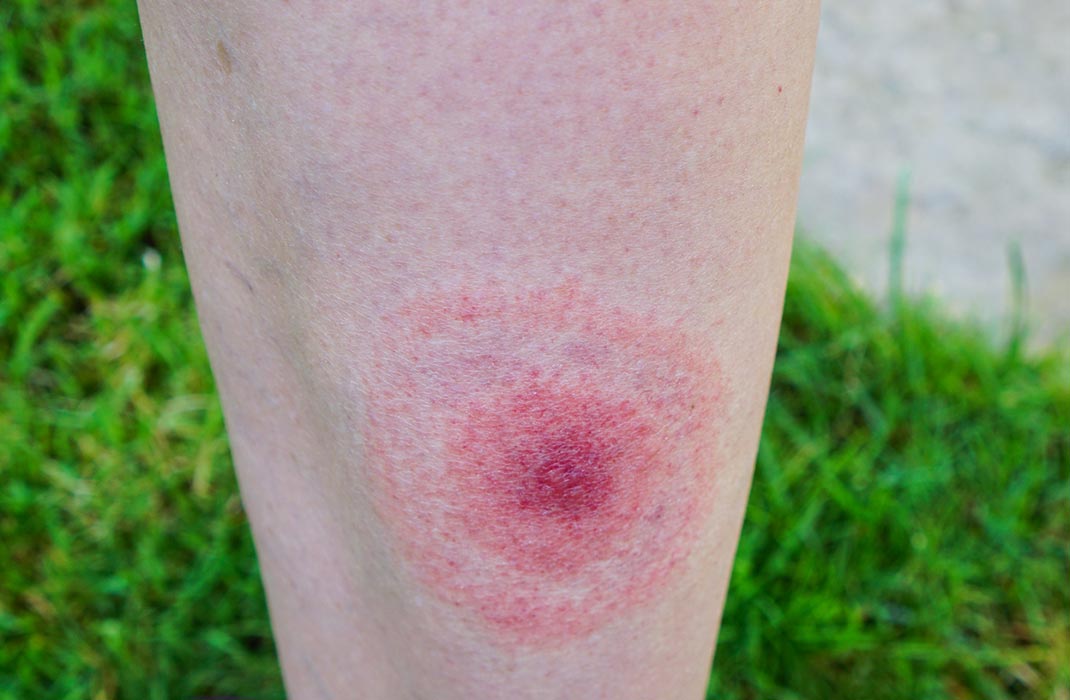
- Lyme disease
- Ringworm
- Hand, foot, and mouth disease
- Fifth disease
- Athlete’s foot

Contributor
Contributor
Related articles
-

published on
-

published on
-

published on
-

published on
-

published on
-

published on
-

published on
-

published on
-
published on